ADVANCED WOMEN’S IMAGING IS NOW OFFERING A RANGE OF OPTIONS FOR NIPT (HARMONY, GENERATION, PANORAMA)
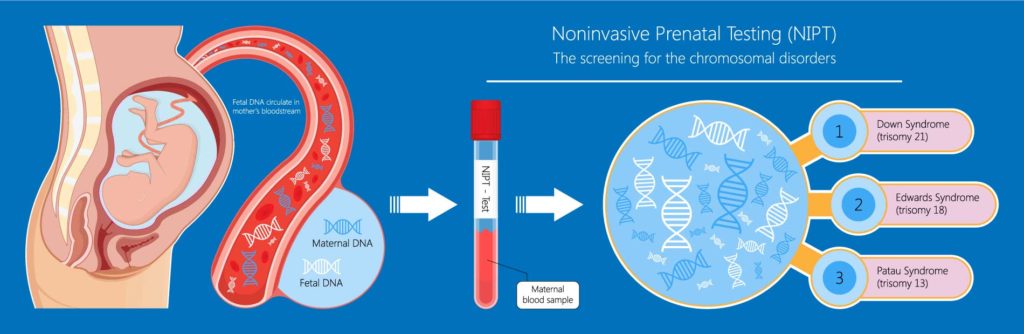
Harmony, Generation and Panorama are different types of non-invasive prenatal tests (NIPT). They assess blood from the mother, looking at the baby’s DNA in her blood (analyses maternal serum for fetal DNA).
It provides limited screening for chromosomes 21, 13, 18 and/or XY (sex chromosomes).
NIPT has a higher detection rate for trisomy 21 than combined first trimester screening (nuchal translucency scan plus maternal serum screening).
NIPT identifies:
- 99% of the fetuses with trisomy 21 (Down syndrome)
- 97% of fetuses with trisomy 18 (Edwards syndrome)
- 92% of fetuses with trisomy 13 (Patau syndrome)
NIPT with Harmony, Generation or Panorama should be seen as an advanced screening test rather than a diagnostic test. It does not detect all cases of trisomy 21, 18 or 13.
NIPT also has a lower false positive rate than combined first trimester screening. This means that less women will need either chorionic villus sampling or amniocentesis to confirm a high risk result, when they actually have a normal baby unaffected by a chromosome problem. This exposes less women to the risk of miscarriage, since both chorionic villus sampling and amniocentesis are associated with a risk of miscarriage secondary to the procedure.
NIPT is a simple blood test with no risk to the fetus.
Testing for microdeletions including 22q 11.2 (Di George syndrome), Angelman syndrome, Prader-Willi syndrome and Cri-Du-Chat syndrome is also available with some forms of NIPT.
NIPT is usually performed after 10-12 weeks of gestation. It can be performed in both single and twin pregnancies, as well as IVF pregnancies.
NIPT can be performed at any stage during the pregnancy after 10 weeks gestation, especially if there are concerns raised after your morphology ultrasound at 18-20 weeks that increase your risks for trisomy 21, trisomy 18 or trisomy 13.
There are 2 ways that NIPT is commonly used in Australia:
- as a first line investigation. This means you have NIPT first (for example, at 10-12 weeks gestation) and then come back for the nuchal translucency ultrasound / first trimester screening at 13 weeks gestation.
- as contingency screening. This means you have the nuchal translucency ultrasound / first trimester screening first and then decide on the need for further testing depending on your adjusted risks. You may then opt to have either NIPT or prenatal diagnostic testing with CVS/amniocentesis, depending on how much additional information you desire about the baby’s chromosomes.
Our doctor will contact you directly once the results of NIPT have returned. This usually takes 7-14 days.
Sometimes the initial sample of your blood may not give a result. This is often related to technical factors and does not mean there is a problem with your baby. It is more likely to occur if you are earlier in your pregnancy (such as 10 weeks gestation, rather than 13 weeks gestation) or due to factors such as increased maternal weight. If this happens, we will call you to organize the collection of another sample of your blood, at no additional cost. For most patients, this repeat sample will give a result.
If the NIPT shows a “high risk” or “aneuploidy detected” result for a chromosome problem involving chromosomes 21, 13, 18, X or Y, this does not mean that your baby definitely has one of these defects. NIPT is not a diagnostic test, and for each of these chromosomes tested, there is a possibility that the result is incorrect (called the “false positive rate”). We recommend an ultrasound to assess your baby for possible structural abnormalities that may support a diagnosis of a chromosome problem, and then discuss the need for diagnostic testing with either chorionic villus sampling or amniocentesis to confirm this diagnosis before making decisions about your pregnancy.
If NIPT shows a “low risk” or “no aneuploidy detected” result, this means your baby is unlikely to have a chromosome problem involving chromosomes 21, 13, 18, X or Y. But NIPT does not detect all cases of chromosome abnormalities or genetic defects.
If ultrasounds of your baby detect structural abnormalities or other concerning features, your doctor may suggest additional testing such as amniocentesis, even if the results of NIPT were reassuring.
NIPT does not give information on other chromosomal abnormalities or genetic problems.
If your 11-13 ultrasound shows an increased nuchal translucency (more than 3.5 mm) or major defects involving the baby’s heart, brain or other organs, the risk for a less common chromosome problem will increase. If this happens, your doctor may suggest you have chorionic villus sampling or amniocentesis.
NIPT does not give information on physical or structural problems with your baby, such as heart or brain abnormalities, and it does not assess the growth or size of your baby.
It is recommended that NIPT be used in conjunction with nuchal translucency ultrasound/first trimester screening, rather than considering the tests as an either/or scenario.
Both NIPT and nuchal translucency ultrasound assess your risks for trisomy 21, trisomy 18 and trisomy 13, but there are significant advantages to having both tests performed.
The nuchal translucency ultrasound / first trimester screening is commonly perceived as “just a test looking for Down syndrome”.
But in reality, nuchal translucency ultrasound / first trimester screening is much more than this.
The nuchal translucency ultrasound also assesses the structure/anatomy of your baby, meaning that you do not need to wait until 18- 20 week morphology ultrasound for an initial assessment of your baby’s anatomy. Many anatomical abnormalities can be diagnosed in the first trimester with careful ultrasound, and may potentially alter the management of your pregnancy. The amount of information gained about the baby’s anatomy at this early gestation will often depend on the level of skill and experience of the person performing the ultrasound. This scan will also review the thickness of the nuchal translucency, for if the nuchal translucency measurement is more than 3.5mm, there is an increased risk of another chromosome abnormality in your baby, other than trisomy 21, trisomy 18 or trisomy 13. NIPT would then not be considered sufficient for the assessment of your baby and your doctor would discuss the option of prenatal diagnostic testing with CVS or amniocentesis for definitive (100%) diagnosis of all the baby’s chromosomes.
First trimester serum screening is also still useful because it assesses the risks of your pregnancy developing complications related to the placenta, such as intrauterine growth restriction. If you are considered at increased risks because your PAPP-A is low, your pregnancy may require extra ultrasounds in the third trimester to monitor the growth and well-being of your baby.
It is therefore recommended that, in addition to NIPT, you have ultrasounds of your baby at 11-13 weeks (nuchal translucency ultrasound including first trimester maternal serum screening with free BhCG and PAPP-A) and at 18-20 weeks to examine the fetal anatomy.
Advanced Women’s Imaging offers a range of NIPT options. The cost of NIPT depends on the type of NIPT performed and can be discussed when booking your appointment.
Your appointment for NIPT includes a brief ultrasound to confirm that your baby is the correct size/dates and has a heart-beat; counselling about the use of NIPT in your pregnancy; collecting the blood sample and sending the sample to the laboratory for analysis; and communication of the results to you and your doctor.
The cost of your appointment does not include detailed ultrasound of your pregnancy, which may also be requested by your doctor.
NIPT itself is not rebated by Medicare however you will receive a rebate for both the ultrasound confirming viability and dates, and the consultation that occurs at the time of your appointment (rebate is approximately $90-100).
You will need an appointment at Advanced Women’s Imaging for NIPT.
Phone our friendly reception staff on 5436 7550 to organize an appointment.
If you have questions about the test or the results of previous ultrasounds, please advise our reception staff. If needed, our doctor can talk to you about the test prior to your appointment.
You do not need a referral to have NIPT, but it is preferable if you have spoken with your doctor about the test and its suitability for you.
You will need a referral from your doctor if you need ultrasounds with Advanced Women’s Imaging prior to having NIPT (including dating ultrasounds, second opinion ultrasounds, nuchal translucency ultrasounds). You will also need a referral if you wish to be eligible for the rebate associated with dating/viability ultrasound prior to NIPT.
NIPT is a good test for many women, but it is not suitable for everyone.
Many woman will benefit from ultrasounds (including second opinion ultrasounds) and counselling at Advanced Women’s Imaging before proceeding with NIPT.
Some women will need to have chorionic villus sampling or amniocentesis rather than NIPT, if there are increased concerns about the baby having a chromosome problem.
